What is TARE (transarterial radioembolisation)?
TARE (transarterial radioembolisation) is a treatment for liver cancer, and liver metastases. It is the delivery of very small spheres (microspheres) with a radioactive substance inside directly into the cancerous tissue through the arteries feeding the tumour.
A radioactive substance called yttrium-90 (Y90) is used in TARE therapy. When treating a tumour by radiation, the surrounding healthy tissue is protected. As with other types of radiation therapy, the radioactive substance used in the treatment does not pass through healthy parts of the body to reach the cancer cells.
What is TARE done for?
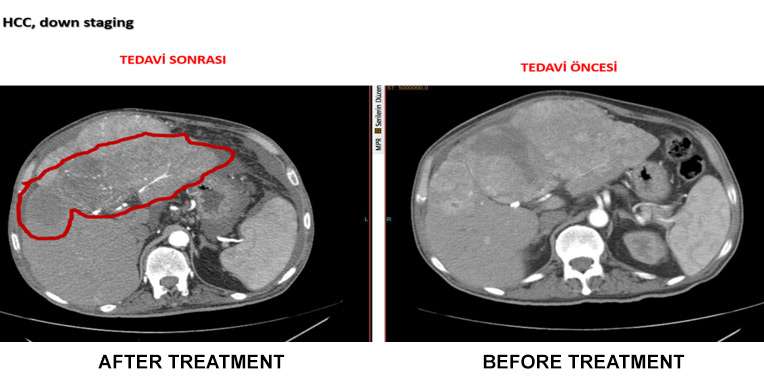
- The treatment reduces the liver tumour, making the patient suitable for surgery.
- It kills cancer cells, allowing the patient to gain time for organ transplantation.
- Shrinks tumour unsuitable for organ transplantation, providing the patient with a chance for a transplant.
- It provides a treatment option for patients for whom chemotherapy is ineffective.
- It helps relieve symptoms.
How does the process of preliminary TARE progress?
Based on an interdisciplinary approach to TARE treatment, the decision is made by a council that includes departments of oncology, nuclear medicine, interventional radiology, general surgery, gastroenterology, and pathology.
Pre-treatment angiography allows to calculate which vessel is feeding the liver tumour, whether there are any leaks to other abdominal organs, the presence of a shunt to the lungs and the dose of Y90 microsphere to be administered to the patient.
How long will TARE take?
The TARE treatment typically within 10-15 days following angiography. The procedure may take between 1 and 3 hours. The duration varies depending on the number of tumours and their location.
After the treatment procedure, the patient is observed in the hospital for 1 night and is discharged the following day based on blood test results. The patient is called in for an examination within 7 to 10 days later and the response to treatment is assessed using CT, MRI, and/or PET/CT scans, as well as laboratory tests after 5 months of administration.
When using TARE, treatment is administered to only one lobe of the liver at a time. Therefore, if treatment is required in another liver lobe, re-planning is carried out. The TARE stages to be administered for the other lobe are the same as for the previous one.
Lutetium-177 treatment is administered in the form of Lu-177 PSMA for prostate cancer and Lu-177 DOTA for neuroendocrine tumours.
Lu-177 PSMA therapy is used for treating prostate cancer that has spread throughout the body and become resistant to other treatment methods. Recently developed medications (such as enzalutamide and abiraterone) year by year helps to extend survival time for the prostate cancer patient. However, resistance to these next-generation treatments develops within 1-2 years, and after this stage, the survival time significantly decreases. At this complex stage of prostate cancer treatment, Lu-177 PSMA therapy aims to reduce the size and progression of the cancer, alleviate symptoms, and maintain and improve quality of life while doing so.
Lu-177 PSMA therapy is determined based on the collection of Ga-68 PSMA PET/CT images. It has been found that if the Ga-68 PSMA PET/CT is positive, indicating abnormalities in metastatic areas and the primary tumour bed, Lu-177 PSMA therapy can be applied. After Lu-177 PSMA treatment, the patient can be discharged on the same day. There are no serious side effects.
LUTETIUM-177 TREATMENT COURSE
Lutetium-177 treatment is typically administered every 6-8 weeks. The total number of treatment courses can vary depending on the patient’s prior treatment and response to therapy. Usually, no less than 2 procedures are conducted. After two courses of treatment, the cancer’s response to therapy is assessed using PET/CT visualization with gallium-68. This visualization helps evaluate the treatment response.
Actinium-225 therapy is used in the form of actinium-225 PSMA for prostate cancer and actinium-225 DOTA for neuroendocrine therapy.
Actinium-225 PSMA therapy is used for treating prostate cancer that has spread throughout the body and become resistant to other treatment methods. At this incurable stage of prostate cancer, actinium-225 PSMA therapy aims to reduce the tumour size and progression of the cancer, alleviate symptoms, and also maintain and improve quality of life.
ACTINIUM-225 TREATMENT COURSE
Actinium-225 treatment is typically administered every 6-8 weeks. The total number of treatment courses can vary depending on the patient’s prior treatment and response to therapy. Usually, no less than 2 procedures are conducted. After two courses of treatment, the cancer’s response to therapy is assessed using gallium-68 PET/CT visualization. The visualization results are used to evaluate the response to treatment.

What is radioactive iodine and how does it treat?
Radioactive iodine is used for treating thyroid cancer and toxic goitre (hyperthyroidism). Administered in the form of capsules or liquid orally, it is absorbed from the gastrointestinal tract and accumulates in the thyroid cells, destroying unwanted thyroid tissues through its emitted radiation. In layman’s terms, this is decommunization, also known as atomic therapy.
How and for how long is radioactive iodine eliminated from the body?
A significant portion of the iodine taken in is retained by the thyroid gland. The iodine contained in other parts of the body is present in small amounts and does not harm tissues. Radioactive iodine is primarily excreted from the body through urine, and some through saliva, sweat, and faeces. On the other hand, the part that is not excreted from the body spontaneously disappears after a while; approximately after 1 month, there will be no radiation left in the body.
Transarterial chemoembolization (TACE) is an interventional radiological treatment for tumours that are localised only in the liver. Based on a multidisciplinary approach to TACE treatment, a council consisting of departments of oncology, nuclear medicine, interventional radiology, and general surgery decides on the application of TACE. TACE is a treatment that is known to be more effective than chemotherapy alone. It does not interfere with chemotherapy and can be administered alongside it.
During the TACE process, a cancer medication is injected into the liver’s vein and into the tumour, along with special plugs that block tumour vessels. Its most significant advantage is that it directly blocks the tumour vessels, preventing the tumour from receiving nourishment. The cancer medication administered via TACE remains in the tumour longer. A day hospitalisation may be required after the procedure. The procedure has a low complication rate and is a comfortable treatment option for patients. If necessary, treatment can be repeated, typically 1-3 months after initial treatment.
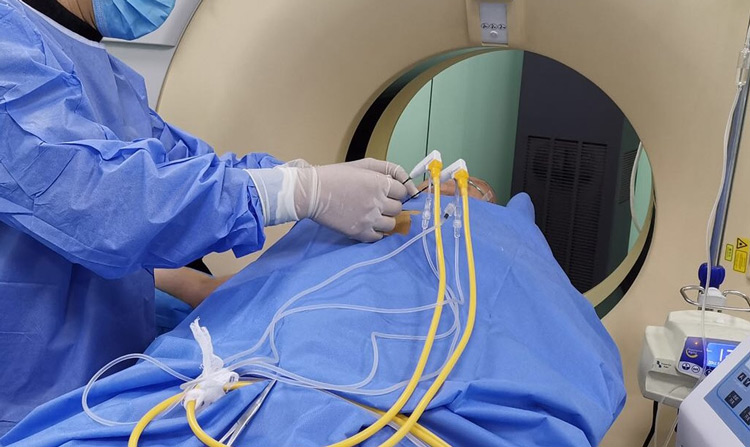
Radiofrequency and microwave therapy is the process of inserting a needle into a soft tissue tumour, forming a mass, and destroying this mass with radiofrequency and microwave energy (mainly thermal energy). This is the destruction of the tumour by burning with radiofrequency and microwave energy. Another method similar to them is cryoablation. In the cryoablation method, the tumour is destroyed by cryo-preservation. In average, a day hospitalisation may be required after the procedure.
WHICH TUMOURS ARE SUBJECT TO RADIOFREQUENCY, MICROWAVE AND CRYOABLATION TECHNIQUES?
- Radiofrequency, microwave and cryoablation techniques are used in tumours that meet avi criteria.
- They are most often used for liver tumours, less often for kidney, lung and bone tumours treatment.
- Sometimes they can also be used for tumour recurrence after surgery.
- Tumour treatment (ablation) using radiofrequency and microwaves is as effective as surgical removal of the tumour, especially for liver tumours smaller than 3 cm.